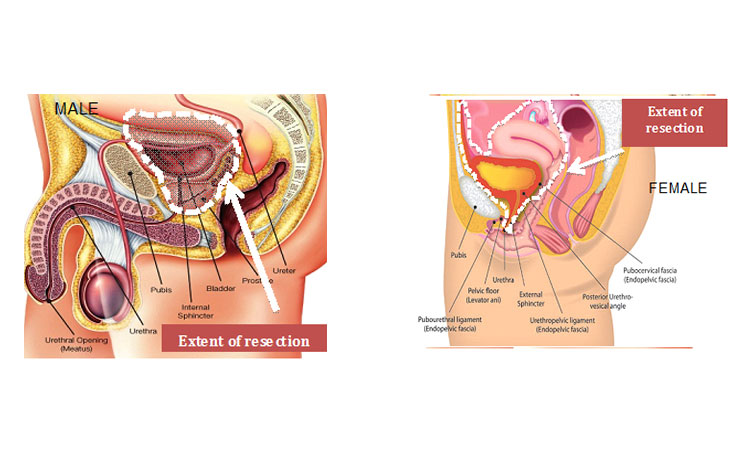
Although with laparoscopic and robotic cystectomy the blood loss is quite minimal we tend to request a few units of blood in case you require a blood transfusion either during or after the operation.
You are likely to be admitted the day before surgery. You may be asked to maintain a mainly fluid diet on this day. You are likely to get an enema that evening and another one the following morning prior to surgery. You will be fasting from midnight (if surgery is scheduled for the morning) and will be having an intravenous ‘drip’ running to keep you well hydrated.
You will be fitted for some special stockings (thrombo-embolic deterrent – TED). These prevent you from developing clots (deep vein thrombosis – DVT) in your legs. You will need to wear these before being taken to the operating rooms. You will also receive injections of heparin following the operation to protect against DVT. I generally advise my patients to wear TED stockings for a period of 4 – 6 weeks after RC.
What happens after the operation?
You will be shifted to ICU for post-op care for a period of 24-48 hours. This is standard practice. In addition to ‘drips’ running into your neck, these lines help monitor your heart condition. You will also have a tube running through your nose into your stomach (nasogastric or NG tube) to keep it empty. Fluid diet may be given through this tube after the operation – this practice varies from hospital to hospital.
Depending on the type of urinary diversion done you are likely to have additional catheters / tubes. If you have had an ileal conduit, urine will be draining into a urostomy bag.
You are likely to be allowed small sips of fluids soon after the operation. As the bowel gets very lazy after this kind of a major operation, solid diet is introduced only after resumption of bowel activity. The sign of this is passing wind / gas through the back passage (flatus). This may take 3-4 days. There is some evidence to suggest that chewing gum in the post-op period may be helpful.
It is very important to start mobilizing as soon as is physically possible. This aids in all aspects of early recovery. A physiotherapist will help you with deep breathing and coughing exercises to protect against developing chest infection. The drips and the various tubes are likely to be removed in a phased manner over the ensuing few days. The join between the ureters and bowel is protected by ‘stents’ that are likely to remain in place for a few weeks. They will be removed at the appropriate time or you may be advised about them ‘falling out’ on their own.
Recovery is rapid following laparoscopic or robotic radical cystectomy, as the cuts made are very small and blood loss is minimal.
What effects will the operation have on my sex life?
Men
Erections
This operation interferes with potency with 50% of men having long-term difficulty. Better results occur in younger men who were sexually active. All men are impotent immediately after the operation. Potency may return after 2 years but some men will remain impotent. There are a number of methods to allow impotent men to achieve erections. These include the use of medications like Viagra. Please discuss this further at your follow-up appointment.
Ejaculation
You can still experience an orgasm but you will not ejaculate any fluid.
Fertility
You will be infertile.
Women
Vaginal bleeding
You will no longer have periods if you were having them before the operation.
Hot flushes
If you have not been through the menopause, you will experience hot flushes and other symptoms associated with removal of the ovaries. Significant symptoms may be helped by hormone replacement therapy.
Penetration
Your vagina may be smaller following the operation. In addition you may experience some dryness, which can be helped by the use of lubricants.
Orgasms
You should still experience orgasms. However as the vagina has a healing wound and may be tighter than before the operation, intercourse may not be pleasurable until everything has healed and the vagina is no longer sore.
What are the long-term effects of the operation?
Benefits: Potential cure of bladder cancer
Potential Problems:
Need to revise the conduit / stoma
Narrowing of the stoma or bleeding from it
Incontinence (neobladder)
Stones (catheterisable pouch / neobladder)
Recurrent urinary infections
Sexual problems as outlined above
My urologist has offered me laparoscopic / robotic RC. Could you please tell me why this is better than the standard open RC?
With the minimally invasive options – lap or robotic RC – the advantages are: